Genetics
Abstract
Osteofibrous dysplasia (OFD) is a skeletal RASopathy presenting with periosteal bone lesions that may progress to fracture and delayed healing (pseudarthrosis). MET gene mutations reducing ubiquitin-mediated protein degradation via loss of the juxtamembrane domain (METΔJMD) were previously identified in OFD patients, resulting in ligand-dependent gain-of-function. The impact of METΔJMD expression on skeletal progenitor cell differentiation and the potential efficacy of targeted therapies remain unclear. We engineered MetΔJMD mice and showed that MetΔJMD expression inhibited osteogenic differentiation of skeletal progenitor cells in vitro and impaired cortical bone development and reduced bone stiffness in vivo. In contrast, conditional deletion of Met enhanced osteogenic differentiation of periosteal progenitor cells. Inhibition of MAPK signaling with MEK inhibitors restored osteogenic differentiation of mouse MetΔJMD skeletal progenitor cells and promoted activation of transcriptional signatures associated with skeletal development and osteoblast differentiation in OFD patient pseudarthrosis-derived primary cells. With this preclinical support, we treated with the MEK inhibitor mirdametinib a pediatric OFD patient suffering from a 3-year history of persistent pseudarthrosis, resulting in fracture union. Our findings demonstrate a bi-directional role for MET in regulating osteogenic differentiation of skeletal progenitor cells and a therapeutic avenue to improve clinical outcomes for this, and potential other, skeletal RASopathies.
Authors
Aysha Khalid, Kristin Denton, Nandina Paria, Ila Oxendine, Meghan Wassell, Reuel Cornelia, Sasidhar Uppuganti, Jeffry S. Nyman, G. Jayashree Jagadeesh, Carlos R. Ferreira, Simon J. Conway, Robert E. Hammer, John O. Ritter, Mylinh Nguyen, David A. Podeszwa, Laura J. Klesse, Carol A. Wise, Jonathan J. Rios
Abstract
SLC13A5 citrate transporter disorder is a rare epileptic encephalopathy caused by loss of function pathogenic variants in the SLC13A5 gene. Loss of sodium/citrate cotransporter (NaCT) function causes a severe early life epilepsy resulting in life-long developmental disabilities and increased extracellular citrate. Current antiseizure medications may reduce seizure frequency, yet more targeted treatments are needed to address the epileptic and neurodevelopmental SLC13A5 phenotype. We performed preclinical studies in SLC13A5 deficient mice evaluating phenotype rescue with adeno-associated virus (AAV) vector carrying a functional copy of the human SLC13A5 gene (AAV9/SLC13A5). Cerebrospinal fluid-delivery of AAV9/SLC13A5 decreased extracellular citrate levels, normalized electrophysiologic and sleep architecture abnormalities, and restored resistance to chemically induced seizures and death. Treatment benefits were achieved with administration during early brain development and in young adult mice, indicating therapeutic efficacy across developmental and post-developmental stages. Comparison of delivery routes in young adult KO mice showed that higher brain targeting achieved with intra-cisterna magna delivery resulted in greater treatment benefit as compared to intrathecal lumbar puncture delivery. Together, these results support further development of AAV9/SLC13A5 for treating SLC13A5 citrate transporter disorder.
Authors
Lauren E. Bailey, Raegan M. Adams, Morgan K. Schackmuth, Irvin T. Garza, Krishanna Knight, Sydni K. Holmes, Meghan M. Eller, MinJae Lee, Rachel M. Bailey
Abstract
Mutations in SLC26A4 are the second most common cause of hereditary hearing loss in many Asian countries, leading to DFNB4, a condition characterized by progressive hearing loss and inner ear malformations. While gene therapy holds great potential, its postnatal application has remained unexplored due to the lack of suitable animal models and the challenges of prenatal intervention. This study represents the first preclinical investigation of postnatal gene therapy for DFNB4 using a clinically relevant Slc26a4 mutant mouse model that closely replicates human auditory phenotypes. Utilizing the synthetic AAV.Anc80L65 vector, we achieved robust SLC26A4 delivery to critical cochlear regions, including the endolymphatic sac and cochlear lateral wall. Comprehensive phenotypic analyses revealed a critical therapeutic window spanning the neonatal and juvenile stages, within which AAV.Anc80L65-mediated SLC26A4 delivery significantly improved hearing, as evidenced by lower auditory brainstem response thresholds. Moreover, the therapy preserved hair cells, reduced endolymphatic sac enlargement, partially restored the endocochlear potential, and mitigated inner ear structural degeneration. These therapeutic effects persisted into adulthood, highlighting the long-term efficacy of postnatal gene therapy. Together, these findings establish a critical therapeutic window for DFNB4 and demonstrate the feasibility of targeting the endolymphatic sac and cochlear lateral wall for effective intervention.
Authors
Yi-Hsiu Tsai, Peng-Yu Wu, Yu-Chi Chuang, Chun-Ying Huang, Hiroki Takeda, Hiroshi Hibino, Chen-Chi Wu, Yen-Fu Cheng
Abstract
SEL1L is a well-known protein in the ER-associated degradation (ERAD) pathway. While it is known to be expressed in platelets, SEL1L has never been shown to play an active role. Here, we present evidence that SEL1L regulates platelet function. We first identified SEL1L through the study of Atypical Equine Thrombasthenia (AET), an autosomal recessive platelet disorder found in thoroughbred horses. A missense variant in SEL1L (c.1810A>G p.Ile604Val) was found in AET-affected horses, which we show is associated with decreased protein expression. SEL1L is intracellular in equine platelets and localizes to the surface upon activation with thrombin. Platelets from homozygous horses exhibited substantially decreased spreading on immobilized collagen. Human megakaryocytes were found to have 2 SEL1L protein isoforms that increase in expression during megakaryopoiesis, although only 1 isoform was delivered to mature platelets. Studies using inducible mouse and constitutive zebrafish KOs demonstrated that SEL1L is necessary for efficient platelet or thrombocyte (fish equivalent) adhesion to sites of endothelial injury. These data reveal a previously undescribed and conserved role for the ERAD pathway in the etiology of AET and platelet function, and GWAS data suggest that it may play a role in human platelet disorders as well.
Authors
Anna R. Dahlgren, Francesca Careddu, Jeffrey W. Norris, Christian A. Di Buduo, Livia Stanger, Reheman Adili, Erin M. Kropp, Qing Li, Michael Holinstat, Ida Biunno, Alessandra Balduini, Fern Tablin, Jordan A. Shavit, Carrie J. Finno
Abstract
Authors
Stephen G. Kaler
Abstract
Authors
Vishal M. Gohil, Michael J. Petris, Francesc Palau
Abstract
BACKGROUND. MASLD has a substantial inherited component. Rare variants in Apolipoprotein B gene (APOB) have been implicated in susceptibility to liver steatosis, but their role in disease progression and outcomes is unclear. METHODS. We investigated APOB rare variants in a case-control cohort of people with advanced MASLD vs. healthy controls (n = 510/261), a family-based study (n = 43 and literature meta-analysis), the Million Veteran Program cohort (MVP, n = 94,885) and the UK Biobank (UKBB, n = 417,657). RESULTS. In the clinical cohort, APOB variants were enriched in people with advanced MASLD (OR 13.8, 95% c.i. 2.7-70.7, P = 0.002) and associated with lower circulating lipids, but higher MASLD activity and fibrosis (P < 0.05). In the family study, APOB variants segregated with hepatic steatosis and fibrosis (P < 0.05). Cross-ancestry meta-analysis of the study cohorts yielded pooled ORs for cirrhosis and hepatocellular carcinoma of 1.82, 95% c.i. 1.33-2.49 and 3.53, 95% c.i. 2.09-5.98, respectively. Variants affecting specifically ApoB100 had a three-fold greater impact on hepatic lipid metabolism compared to those impairing also ApoB48 and were specifically protective against coronary artery disease (P < 0.05). Variants affected cirrhosis risk similarly, but ApoB48/100 had a larger impact on hepatocellular carcinoma (P < 0.05). CONCLUSIONS. Rare APOB variants predispose to advanced MASLD and HCC, with distinct contributions from disrupted VLDL and chylomicrons secretion. These findings highlight the interplay between hepatic and intestinal lipid handling, suggesting that APOB genotyping may enhance MASLD risk stratification and case identification. FUNDING. European Union, Italian Ministry of Health, Swedish Research Council, Veteran health administration, NIH.
Authors
Matteo Mureddu, Serena Pelusi, Oveis Jamialahmadi, Marijana Vujkovic, Lorenzo Miano, Hadi Eidgah Torghabehei, Luisa Ronzoni, Francesco Malvestiti, Marco Saracino, Giulia Periti, Vittoria Moretti, Craig C. Teerlink, Julie A. Lynch, Philip S. Tsao, Josephine P. Johnson, Vincenzo La Mura, Robertino Dilena, Saleh A. Alqahtani, Alessandro Cherubini, Francesco Paolo Russo, Roberta D'Ambrosio, Mirella Fraquelli, Salvatore Petta, Luca Miele, Umberto Vespasiani-Gentilucci, Elisabetta Bugianesi, Rosellina M. Mancina, Paolo Parini, Daniele Prati, Kyong-Mi Chang, Carolin V. Schneider, Stefano Romeo, Luca V.C. Valenti
Abstract
Cervical cancer (CC) remains the fourth leading cause of cancer-related deaths in women globally, with poor prognosis for metastatic and recurrent cases. Although genomic alterations have been extensively characterized, global proteogenomic landscape of the disease is largely under-explored. Here, we present the first genome-wide proteogenomic characterization of CC, analyzing 139 tumor-normal tissue pairs using whole-genome sequencing, transcriptomics, proteomics, and phosphoproteomics. We identified four distinct molecular subtypes with unique clinical outcomes: epithelial-mesenchymal transition (EMT, C1), proliferation (C2), immune response (C3), and epithelial differentiation (C4). A four-protein classifier (CDH13, TP53BP1, NNMT, HSPB1) was developed with strong prognostic and predictive value, particularly for immunotherapy response in subtype C3. Phosphoproteomic profiling uncovered subtype-specific kinase activity, identifying actionable therapeutic targets. Our findings further revealed previously uncharacterized somatic copy number alterations, extrachromosomal DNA landscape, and human-HPV fusion peptides, with implications for genetic heterogeneity and therapeutic targets. This study enhances the understanding of cervical cancer through deeper proteogenomic insights, and facilitates the development of personalized therapeutic strategies to improve patient outcomes.
Authors
Xun Tian, Mansheng Li, Zhi Wang, Tian Fang, Yi Liu, Jin Fang, Lejing Wang, Zhichao Jiang, Xingyu Zhao, Chen Cao, Zhiqiang Yu, Meiying Yang, Songfeng Wu, Yifan Wu, Rui Tian, Hui Wang, Yunping Zhu, Zheng Hu
Abstract
Ceramides are essential skin lipids for maintaining the mammalian skin permeability barrier, which protects against external stimuli. The precursor of epidermal ceramides, glucosylceramides (GlcCer), is synthesized within granular keratinocytes while its precise cellular transport mechanisms remain poorly characterized. Here, we identified three pathogenic variants in the GLTP gene, which encodes glycolipid transfer protein, in five unrelated families with nonsyndromic epidermal differentiation disorder presenting with generalized skin scaling. The biallelic GLTP variants resulted in loss of competent GLTP expression. CRISPR/Cas9-generated Gltp knockout mice exhibited lethal barrier defects, partially recapitulating the clinical features of our patients. We demonstrated that GLTP facilitated GlcCer transport in differentiated keratinocytes, with its deficiency causing impaired GlcCer trafficking and consequent aberrant retention in lysosomes, thereby disrupted lysosome function. The lysosomal dysfunction impaired autophagy flux, resulting in delayed keratinocyte terminal differentiation, which is expected to compromise the skin barrier integrity and ultimate abnormal scaling. Pharmaceutical inhibition of GlcCer synthesis effectively rescued both autophagy and keratinocyte differentiation defects. Our findings establish GLTP as a novel underlying gene for nonsyndromic epidermal differentiation disorders and unravel its essential role in maintaining skin homeostasis during terminal differentiation by mediating epidermal GlcCer transport.
Authors
Zeqiao Zhang, Shimiao Huang, Adam Jackson, Elizabeth A. Jones, Siddharth Banka, Chao Yang, Sisi Zhao, Kunlun Lv, Sha Peng, Zhimiao Lin, Huijun Wang
Abstract
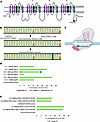
SCN8A encodes the voltage-gated sodium channel Nav1.6, which plays a key role in facilitating neuronal excitability. Mutations in SCN8A, particularly gain-of-function variants, cause SCN8A developmental and epileptic encephalopathy (DEE), a severe epilepsy syndrome characterized by seizures, cognitive dysfunction, movement disorders, and sudden unexpected death in epilepsy (SUDEP). The recurrent SCN8A variant R1872W impairs channel inactivation, causing neuronal hyperexcitability and seizures. Current treatments, including antiseizure medications, are often ineffective for patients with SCN8A DEE, highlighting the need for targeted therapies. We employed base editing to correct the R1872W SCN8A variant. An adenine base editor and guide RNA (SCN8A-ABE) were packaged within dual PhP.eB-adeno-associated viruses (AAVs) and administered to R1872W mice at P2. SCN8A-ABE significantly increased survival of mice expressing R1872W and either reduced seizure incidence and severity or eliminated seizure occurrence. Electrophysiological recordings revealed a rescue of seizure-associated neuronal hyperexcitability and suppression of the pathogenic persistent sodium current (INaP) in treated mice. Comorbidities, including diminished mobility and anxiety-like behaviors, were improved by SCN8A-ABE. These effects were achieved by a 32% absolute reduction in mutant transcripts, accompanied by conversion to SCN8A WT transcripts. Our findings demonstrate base editing as an effective targeted therapeutic approach for SCN8A DEEs by addressing the underlying genetic cause.
Authors
Caeley M. Reever, Alexis R. Boscia, Tyler C.J. Deutsch, Mansi P. Patel, Raquel M. Miralles, Shrinidhi Kittur, Erik J. Fleischel, Atum M.L. Buo, Matthew S. Yorek, Miriam H. Meisler, Charles R. Farber, Manoj K. Patel



Copyright © 2026 American Society for Clinical Investigation
ISSN: 0021-9738 (print), 1558-8238 (online)