Abstract
Preclinical studies suggest beneficial effects of GLP-1 agonists in pulmonary arterial hypertension (PAH). This first-in-disease study evaluated acute hemodynamic effects of GLP-1 agonist, exenatide administered i.v. in patients with idiopathic PAH and CTEPH as well as in a PAH rodent model. Seventeen patients (9 idiopathic PAH) received an exenatide infusion during right heart catheterization, which included multisite sampling for circulating metabolites. Acute effects of exenatide were also assessed by cardiac magnetic resonance imaging in monocrotaline (MCT) PAH and control rats. In the clinical study, exenatide was well tolerated, reduced mean pulmonary artery pressure (45 ± 15 mmHg versus 40 ± 18 mmHg), and improved cardiac index (2.1 ± 0.6 L/min versus 2.4 ± 0.9 L/min/m2) and pulmonary vascular resistance (7.8 ± 8.0 WU versus 5.9 ± 5.0 WU) across all patients. Right ventricular (RV) contractility and afterload improved in a subset of patients undergoing pressure-volume measurements. In an exploratory metabolomics analysis, 47 metabolite levels changed after exenatide infusion, predominantly in free fatty acid pathways. Six metabolites with prognostic relevance in PAH within myocardial glycolytic and lipid oxidation pathways were also altered after exenatide. In MCT rats, exenatide improved RV stroke-volume, RV ejection fraction, and RV-arterial coupling. These findings support the further evaluation of exenatide within chronic studies as a potentially novel pulmonary vasodilator therapy.
Authors
Chinthaka B. Samaranayake, Marili Niglas, Nicoleta Baxan, Alexander Kempny, Ali Ashek, Michael Gatzoulis, Laura C. Price, Konstantinos Dimopoulos, Martin R. Wilkins, Stephen Wort, Christopher J. Rhodes, Lan Zhao, Colm McCabe
Abstract
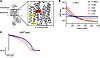
Ischemia/reperfusion (IR) enhances oxidative stress, leading to myocardial injury. Although Perm1 promotes cytoprotective mechanisms, the underlying mechanisms are poorly understood. Cysteine oxidation of Keap1 alleviates Cul3-mediated ubiquitination/degradation of Nrf2 and promotes antioxidant transcription. Here we show that Perm1 activates Nrf2 through cysteine oxidation of Keap1 and stabilization of Nrf2. Endogenous Perm1 was downregulated during IR, whereas the rescue of Perm1 reduced IR injury. Downregulation of Perm1 exacerbated oxidative stress, whereas upregulation of Perm1 alleviated it, accompanied by downregulation and upregulation of Nrf2-regulated antioxidant genes, respectively. Perm1 promoted oxidation of cysteine residues in Keap1, possibly through thiol-disulfide exchange reactions, which decreases Keap1-Nrf2 interaction and inhibits Cul3-mediated degradation of Nrf2. We identified Cys121 and Cys746 in Perm1 as critical for Keap1 oxidation and cardioprotection. Thus, Perm1 induces cysteine oxidation of Keap1, thereby conferring myocardial resistance to IR injury by inducing Nrf2 stabilization and transcriptional activation of antioxidant genes.
Authors
Shin-ichi Oka, Chun-Yang Huang, Masato Matsushita, Allen Sam Titus, Yasuki Nakada, Risa Mukai, Samta Veera, Youssef Mourad, Ghassan Yehia, Peter Romanienko, Yimin Tian, Peiyong Zhai, Junichi Sadoshima
Abstract
Single-ventricle congenital heart disease (SV-CHD) is a uniformly lethal condition requiring the Glenn surgery, which as a side effect eliminates arterial pulsatility and contributes to pulmonary vascular complications. In Glenn patients, we quantified pulsatility loss in each dimension of force (flow, pressure, and stretch) using cardiac catheterization and MRI. To model and investigate the individual impact of each dimension of pulsatility loss on the pulmonary vasculature, we applied isolated pulsatile and non-pulsatile mechanical stimuli to pulmonary artery endothelial cells (ECs) in vitro. We found that each dimension of force triggered distinct transcriptional responses, revealing force-specific regulation of structural and signaling pathways. Pulsatile stretch uniquely stimulated EC secretion of PDGFB, a key driver of vascular smooth muscle cell (vSMC) recruitment. In a rat Glenn model, loss of pulsatility led to vascular wall thinning, loss of EC PDGFB, and reduced activation of smooth muscle PDGFBRβ, confirming in vivo relevance. Our findings uncover a mechanistic link between endothelial stretch sensing and PDGFB-mediated EC-vSMC crosstalk, essential for maintaining pulmonary artery architecture. Clinically, these insights suggest that restoring or mimicking pulsatile forces may help preserve vascular integrity and prevent remodeling in patients with SV-CHD.
Authors
Stephen B. Spurgin, Lauren Thai, Tina C. Wan, Christopher P. Chaney, Mitzy A. Cowdin, Surendranath Veeram Reddy, Tarique Hussain, Munes Fares, M. Luisa Iruela-Arispe, Thomas Carroll, Andrew D. Spearman, Ondine Cleaver
Abstract
Abdominal aortic aneurysm (AAA) lacks effective pharmacological therapies. Here, we investigate transcription factor 7-like 2 (TCF7L2), a genetic locus associated with both thoracic and abdominal aortic aneurysms, to elucidate its role in AAA pathogenesis. Integrating summary-data-based Mendelian randomization (SMR) with single-cell RNA sequencing (scRNA-seq) of human and mouse aortas, we identify TCF7L2 as a gene enriched in vascular smooth muscle cells (VSMCs) and causally linked to AAA development. Smooth muscle cell-specific TCF7L2 knockout significantly attenuates AAA formation across three distinct murine models (Ang II infusion-, BAPN/Ang II co-administration-, and elastase-induced AAA), independent of systemic blood pressure or lipid levels. Mechanistic studies reveal that TCF7L2 directly upregulates MMP14 and downregulates TIMP3 expression in vitro and in vivo, driving MMP2-mediated extracellular matrix (ECM) degradation. Concurrently, TCF7L2 represses integrin β1 (ITGB1) expression, reducing VSMC adhesion to the ECM. Collectively, these findings identify TCF7L2 as a key driver of pathological vascular remodeling in AAA, suggesting that targeting TCF7L2 may offer a novel therapeutic strategy for limiting AAA progression.
Authors
Yongjie Deng, Yaozhong Liu, Yang Zhao, Hongyu Liu, Guizhen Zhao, Zhenguo Wang, Xu Zhang, Chao Xue, Wei Huang, Tianqing Zhu, Haocheng Lu, Yanhong Guo, Lin Chang, Ida Surakka, Y. Eugene Chen, Jifeng Zhang
Abstract
Heterozygous TBX4 variants are the second most common genetic cause of pediatric pulmonary hypertension (PH), yet mechanisms underlying TBX4-related lung disease remain poorly understood. This study developed a lung mesenchyme-specific Tbx4 loss-of-function (Tbx4cKO) mouse model that bypasses embryonic lethality to investigate this condition. Adult Tbx4cKO mice demonstrated significantly impaired pulmonary flow acceleration consistent with PH. Three-dimensional analysis of embryonic lungs revealed reduced lobe volumes and decreased distance between pleural edges and muscularized vessels. In adult Tbx4cKO lungs, we identified extensive vascular remodeling characterized by medial thickening and the extension of muscularized arteries into normally non-muscularized subpleural parenchymal zones. Contrary to previous reports suggesting vascular simplification, three-dimensional analysis demonstrated an elaborated pulmonary artery (PA) tree in addition to pathologic wall muscularization. Depletion of a single Tbx5 allele in addition to both Tbx4 alleles exacerbated histologic phenotypes with worsened right ventricular dilation. This model also demonstrated dysregulated airway smooth muscle patterning and prominent subpleural smooth muscle bands, similar to those in human TBX4 syndrome. We identify TBX4 as a critical regulator of smooth muscle differentiation and patterning across multiple lung compartments. Our model recapitulates key features of human TBX4 syndrome and identifies dysregulated smooth muscle differentiation as a potential future therapeutic target.
Authors
Lea C. Steffes, Kaylie A. Chiles, Sehar R. Masud, Aleen Rahman, Madeline Dawson, Csaba Galambos, Maya E. Kumar, Ripla Arora
Abstract
Aortic dissection (AD) is a catastrophic vascular emergency with high mortality, and current pharmacologic interventions to prevent its progression are limited. Vascular smooth muscle cells (VSMCs) undergo a pathological phenotypic switch from a contractile to a synthetic state during AD, compromising aortic wall integrity; however, the underlying metabolic mechanisms remain poorly understood. In this study, we performed integrative transcriptomic analyses and identified glutaminase 1 (GLS1) as a key regulator of VSMC phenotypic switching in AD. GLS1 expression was significantly downregulated in VSMCs from both human AD aortic tissues and mouse models. Functionally, GLS1 deficiency promoted PDGF-BB–induced VSMC dedifferentiation in vitro. Smooth muscle cells specific Gls1 knockout (Gls1SMKO) mice exhibited aggravated AD upon BAPN treatment, whereas VSMCs specific GLS1 overexpression improved the contractile phenotype and reduced AD incidence. Mechanistically, GLS1 downregulation impaired glutamate metabolism, leading to reduced levels of glutathione and α-ketoglutarate. This metabolic disruption promoted reactive oxygen species accumulation and mitochondrial dysfunction, ultimately triggering VSMC phenotypic switching. Furthermore, we found that GLS1 transcription was repressed by retinoic acid receptor-α (RARα). Pharmacologic inhibition of RARα with AR7 restored GLS1 expression, ameliorated VSMC phenotypic switching, and conferred protection against AD. These findings reveal a critical role of GLS1-mediated glutamate metabolism in VSMC phenotypic switching and suggest a promising therapeutic strategy for AD.
Authors
Wei Xie, Chen Ning, Chen Lu, Dongjin Wang, Shuang Zhao, Tianyu Song, Hailong Cao
Abstract
Increased consumption of ultra-processed foods (UPFs) is a risk factor for metabolic disorders-associated heart failure (HF). Here, we demonstrate that UPF-induced calpain-1 aggravated oxidative stress, thereby increasing high mobility group box 1 (HMGB1)-mediated myocardial inflammation, which contributes to cardiac dysfunction. After illustrating the dysregulated inflammatory pathways in human and murine hearts upon metabolic stress, we revealed an increase in calpain-1 alongside profound oxidative stress and inflammation in the failing myocardium. Mechanistically, in neonatal rat cardiomyocytes (NRCMs) and human induced pluripotent stem cell-derived cardiomyocytes (hiPSC-CMs), HMGB1 was upregulated by calpain-1 and reactive oxygen species (ROS) upon stress of saturated and trans fatty acids (FA). Consequently, HMGB1 promoted a pro-inflammatory response in macrophages. On the contrary, inhibition of calpain or ROS efficiently repressed HMGB1 in cardiomyocytes. Therapeutically, either recombinant adeno-associated virus 9 (AAV9) delivered inhibitor of calpain-1 or its pharmacological inhibitor attenuated ROS and HMGB1-induced inflammation in the myocardium and mitigated HF in both male and female mice fed with an ultra-processed diet (UPD). Collectively, we have demonstrated the effects of suppressing calpain-1 and oxidative stress on alleviating myocardial inflammation via blockage of HMGB1 and cardiac dysfunction. The results provide a promising therapeutic strategy for preventing or treating HF in metabolic disorders.
Authors
Claire Ross, Sanskruti Ravindra Gare, Nasser H. Alatawi, Oveena Fonseka, Xinyi Chen, Jiayan Zhang, Yihua Han, Andrea Ruiz-Velasco, Riham R.E. Abouleisa, Yingjuan Liu, Xiangjun Zhao, Han Xiao, Bernard Keavney, Gareth J. Howell, Tao Wang, Tamer M.A. Mohamed, Elizabeth J. Cartwright, Wei Liu
Abstract
Heart failure with preserved ejection fraction (HFpEF) is a multifactorial disease that develops in several clinical settings. Despite its complex pathogenesis, evidence indicates a central role for fibrosis in the progression of left ventricular (LV) diastolic dysfunction (LVDD). Through exploratory research into brown adipose tissue (BAT)-derived adipokines (BATokines), we identified a secreted-type pro-fibrotic protein, procollagen C-endopeptidase enhancer-1 (PCPE-1), whose expression increased in BAT with aging. PCPE-1 promotes the cleavage of procollagens and is a critical initiator of fibrillogenesis. This molecule was increased in the plasma of aged mice. In addition to aging, dietary obesity led to an increase in PCPE-1 expression in the LV of mice. Both systemic and BAT-specific PCPE-1 depletion ameliorated LV fibrosis and LVDD in the obese HFpEF model. Our data also showed that age-associated LVDD was ameliorated in the systemic PCPE-1 knockout mouse model fed with a normal chow diet. Conversely, the overexpression of PCPE-1 expression in BAT was shown to lead to aggravation of LV fibrosis and LVDD. Mechanistically, we found reactive oxygen species (ROS)/DNA damage/c-Fos/c-Jun signaling resulted in an increased production of PCPE-1 in brown adipocytes. These results indicate PCPE-1 may represent a druggable target for aging- and obesity-related HFpEF.
Authors
Yung-Ting Hsiao, Yohko Yoshida, Hirotsugu Tsuchimochi, Jingyuan Tang, Tin May Aung, Chun-Han Chang, Agian Jeffilano Barinda, Zhihong Li, Nur Syakirah Binti Othman, Tom Yoshizaki, Yiwei Ling, Shujiro Okuda, Manabu Abe, Seiya Mizuno, Satoru Takahashi, Takayuki Inomata, Hidetaka Kioka, Yasushi Sakata, Daichi Maeda, Yuya Matsue, Takaaki Furihata, Hiroshi Iwata, James T. Pearson, Kinya Otsu, Kenneth Walsh, Akihito Ishigami, Tohru Minamino, Ippei Shimizu
Abstract
Short QT syndrome is a heritable arrhythmia disorder linked to sudden cardiac death. We recently identified that individuals with alternating hemiplegia of childhood (AHC), a rare neurodevelopmental disorder, can exhibit shortened corrected QT intervals and elevated risk for ventricular fibrillation. This is especially true for patients with AHC heterozygous for the recurrent ATP1A3-D801N variant, though the underlying cardiac mechanism remains unclear. We hypothesized that the D801N missense impairs Na+/K+-ATPase function, causing Ca2+ overload, shortened action potential duration (APD), and arrhythmias. Using in silico modeling and patient-derived induced pluripotent stem cell cardiomyocytes (iPSC-CMsD801N), we observed shorter APD, elevated intracellular and sarcoplasmic reticulum Ca2+ levels, and delayed afterdepolarizations (DADs) compared with WT. Additionally, increased Ca²+ influx via the Na+/Ca2+ exchanger (NCX1) during depolarization was observed in iPSC-CMsD801N. Simulations and in vitro experiments suggest that reduced ATPase function accelerated inactivation of L-type Ca2+ channels. Pharmacologic inhibition of NCX1 with ORM-10103 normalized APD and reduced DADs. These findings support a Ca2+-mediated mechanism for arrhythmogenesis in ATP1A3-D801N carriers and identify NCX1 as a potential therapeutic target.
Authors
Minu-Tshyeto K. Bidzimou, Padmapriya Muralidharan, Zhushan Zhang, Danyal Raza, Daniel Needs, Bo Sun, Robin M. Perelli, Mary E. Moya-Mendez, P.K. Rakesh Manivannan, Arsen S. Hunanyan, Abbigail Helfer, Christine Q. Simmons, Alfred L. George Jr., Donald M. Bers, Nenad Bursac, Mohamad A. Mikati, Andrew P. Landstrom
Abstract
The RhoBTB1-Cullin3 (CUL3) pathway in smooth muscle cells (SMCs) controls the ubiquitination and proteasomal degradation of target proteins that regulate vasodilation, vasoconstriction, and the actin cytoskeleton, and through this blood pressure (BP) and arterial stiffness. Using proximity labelling coupled with mass spectrometry in A7R5 SMCs, we identified proteins which bound to the C-terminal half of RhoBTB1 which functions as an adapter to deliver substrates to CUL3. We examined the physiological relevance of one of these substrates, RbFox2. Co-immunoprecipitation validated the interaction of RbFox2 with RhoBTB1. RbFox2 expression was elevated in response to inhibition of the ubiquitination-proteasomal pathway, CUL3-deficiency, and RhoBTB1 inhibition by either siRNA or angiotensin II (ANG). RbFox2 was ubiquitinated in a RhoBTB1- and CUL3-dependent manner suggesting its regulation through the RhoBTB1-CUL3-dependent ubiquitin-proteasome pathway. Inhibition of RbFox2 impaired the actin cytoskeleton in A7R5 cells and in primary SMC from RbFox2Flox/Flox (RbFox2F/F) mice and decreased the levels of globular and filamentous actin. ANG increased BP and arterial stiffness of RbFox2F/F mice, but the progression of arterial stiffness was halted after SMC-specific RbFox2 deletion despite a continued rise in BP. We conclude that RhoBTB1 and RbFox2 are important regulators of arterial stiffness through a mechanism that influences cytoskeletal integrity.
Authors
Gaurav Kumar, Nisita Chaihongsa, Daniel T. Brozoski, Daria Golosova, Ibrahim Vazirabad, Ko-Ting Lu, Kelsey K. Wackman, Ravi K. Singh, Curt D. Sigmund
No posts were found with this tag.