Oncology
Abstract
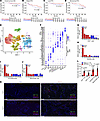
MAP kinase kinase kinase kinase (MAP4K) family kinases are key kinases for T-cell-mediated immune responses; however, in vivo roles of MAP4K2 in immune regulation remain unclear. Using T-cell-specific Map4k2 conditional knockout (T-Map4k2 cKO) mice, single-cell RNA sequencing (scRNA-seq), and mass spectrometry analysis, we found that MAP4K2 interacted with DDX39B, induced forkhead box protein P3 (FOXP3) gene expression, and promoted Treg differentiation. Mechanistically, MAP4K2 directly phosphorylated the DEAD box protein DDX39B, leading to DDX39B nuclear translocation and subsequent Foxp3 RNA splicing. MAP4K2-induced FOXP3 mRNA levels were abolished in DDX39B knockout T cells. Furthermore, T-Map4k2 cKO mice displayed the reduction of Treg population and the sustained inflammation during remission phase of EAE autoimmune disease model. Remarkably, the anti-PD-1 immunotherapeutic effect on pancreatic cancer was significantly improved in T-Map4k2 cKO mice, Treg-specific Map4k2-deficient mice, adoptively transferred chimeric mice, or MAP4K2-inhibitor-treated mice. Consistently, scRNA-seq analysis of human pancreatic patients showed increased MAP4K2 levels in infiltrating Treg cells. Collectively, MAP4K2 promotes Treg differentiation by inducing DDX39B nuclear translocation, leading to the attenuation of antitumor immunity.
Authors
Huai-Chia Chuang, Chia-Wen Wang, Chia-Hsin Hsueh, Yu-Zhi Xiao, Ching-Yi Tsai, Pu-Ming Hsu, Evelyn L. Tan, Hsien-Yi Chiu, Tse-Hua Tan
Abstract
Glioblastoma (GBM) is a highly lethal brain tumor with limited treatment options and resistance to immune checkpoint inhibitors due to its immunosuppressive tumor microenvironment (TME). Here, we identify OLIG2 as a key regulator of immune evasion in GBM stem-like cells, inhibiting CD8+ T cell-dependent antitumor immunity, while promoting pro-tumor macrophages polarization. Mechanistically, OLIG2 recruits HDAC7 to repress CXCL10 transcription, inducing STAT3 activation in tumor-associated macrophages (TAMs) and decreasing CD8+ T cell infiltration and activation. Genetic deletion of OLIG2 significantly increases CXCL10 secretion, shifting TAMs toward an anti-tumor phenotype and enhancing CD8+ T cell activities. Furthermore, upregulated OLIG2 expression is correlated to resistance to immune checkpoint inhibitors (ICIs) in GBM patients. OLIG2 inhibition by either genetic deficiency or pharmacological targeting with CT-179 sensitizes GBM tumors to anti-PD-L1 therapy, enhancing antitumor immune responses and prolonging survival. Our findings reveal OLIG2+ glioma stem-like cells as critical mediators of immune evasion and identify the OLIG2/HDAC7/CXCL10 axis as a potential therapeutic target to enhance immune checkpoint inhibitors efficacy and to improve immunotherapy outcomes in aggressive GBM.
Authors
Xinchun Zhang, Jinjiang Xue, Cunyan Zhao, Chenqiuyue Zeng, Jiacheng Zhong, Gangfeng Yu, Xi Yang, Yao Ling, Dazhen Li, Jiaxiao Yang, Yun Xiu, Hongda Li, Shiyuan Hong, Liangjun Qiao, Song Chen, Q. Richard Lu, Yaqi Deng, Zhaohua Tang, Fanghui Lu
PARP inhibitors restore NK cell function via secretory crosstalk with tumor cells in prostate cancer
Abstract
Prostate cancer (PCa) is one of the most frequently diagnosed malignancies and the main cause of cancer-related death in men worldwide. Poly (ADP-ribose) polymerase (PARP) inhibitors have been approved for the treatment of PCa harboring BRCA1/2 mutations. While the survival benefits conferred by PARP inhibitors (PARPi) may extend beyond this specific patient population based on evidence from recent clinical trials, the underlying mechanisms remain unexplored. Here, we demonstrate that PARPi substantially restore natural killer (NK) cell functions by promoting cyclophilin A (CypA) secretion from PCa cells, which correlates with improved prognosis in PCa patients from our and public cohorts. Mechanistically, tumor-derived CypA specifically from PCa cells binds to ANXA6 and activates the downstream FPR1 signaling pathway, leading to increased mitochondrial oxidative phosphorylation and NK cell activation. Pharmacological inhibition of CypA blocks the FPR1-AKT signaling and diminishes the cytotoxic effects of NK cells, thereby compromising the therapeutic efficacy of PARPi against PCa. Conversely, combining NK cell adoptive transfer therapy with PARPi markedly prolongs survival in mice bearing PCa. Collectively, we reveal a unique secretory crosstalk between PCa cells and NK cells induced by PARPi and propose a promising strategy for treating PCa.
Authors
Zheng Chao, Le Li, Xiaodong Hao, Hao Peng, Yanan Wang, Chunyu Zhang, Xiangdong Guo, Peikun Liu, Sheng Ma, Junbiao Zhang, Guanyu Qu, Yuzheng Peng, Zhengping Wei, Jing Luo, Bo Liu, Peixiang Lan, Zhihua Wang
Abstract
Authors
Johnathan R. Kent, Keene L. Abbott, Rachel Nordgren, Amy Deik, Nupur K. Das, Millenia Waite, Tenzin Kunchok, Anna Shevzov-Zebrun, Nathaniel Christiansen, Amir Sadek, Darren S. Bryan, Mark K. Ferguson, Jessica S. Donington, Alexander Muir, Yatrik M. Shah, Clary B. Clish, Matthew G. Vander Heiden, Maria Lucia L. Madariaga, Peggy P. Hsu
Abstract
Transitions of cancer cells between distinct cell states, which are typically driven by transcription reprogramming, fuel tumor plasticity, metastasis, and therapeutic resistance. Whether the transitions between cell states can be therapeutically targeted remains unknown. Here, using the epithelial-to-mesenchymal transition (EMT) as a model, we show that the transcription reprogramming during a cell-state transition induces genomic instability through R-loops and transcription-replication conflicts, and the cell-state transition cannot occur without the ATR kinase, a key regulator of the replication stress response. ATR inhibition during EMT not only increases transcription- and replication-dependent genomic instability but also disrupts transcription reprogramming. Unexpectedly, ATR inhibition elevates R-loop-associated DNA damage at the SNAI1 gene, a key driver of the transcription reprogramming during EMT, triggering ATM- and Polycomb-mediated transcription repression of SNAI1. Beyond SNAI1, ATR also suppresses R-loops and antagonizes repressive chromatin at a subset of EMT genes. Importantly, inhibition of ATR in tumors undergoing EMT reduces tumor growth and metastasis, suggesting that ATR inhibition eliminates cancer cells in transition. Thus, during EMT, ATR not only protects genome integrity but also enables transcription reprogramming, revealing that ATR is a safeguard of cell-state transitions and a target to suppress tumor plasticity.
Authors
Parasvi S Patel, Jacob P. Matson, Xiaojuan Ran, Marcello Stanzione, Ajinkya S. Kawale, Mingchao Wang, Sneha Saxena, Conrad Sander, Jacquelyn Curtis, Jessica L. Hopkins, Edmond Wong, Ryan B. Corcoran, Daniel A. Haber, Nicholas J. Dyson, Shyamala Maheswaran, Lee Zou
Abstract
Immunotherapy has been effective in many cancer types but has failed in multiple clinical trials in prostate cancers, with the underlying mechanisms remaining largely unclear. Here, we demonstrate that androgen receptor pathway inhibitor (ARPI) plus irradiation (IR) triggered robust anticancer immunity in prostate cancers in both patients and mice. We show that androgen-activated AR suppressed innate immune signaling by inducing inhibitor of nuclear factor kappa-B kinase subunit epsilon (IKBKE) gene repression through HDAC2 interaction with an IKBKE enhancer RNA (IKBKE eRNA, or IKBKE-e). ARPI treatment caused IKBKE derepression and enhanced an IR-induced innate immune response via action of RIG-I and MDA5 dsRNA sensors. IKBKE-e ablation largely enhanced innate immunity in prostate cancer cells in culture and anticancer immunity in mice. Our results revealed AR, HDAC2, and IKBKE eRNA as critical intrinsic immune suppressors in prostate cancer cells, suggesting that rejuvenating inhibitor of nuclear factor kappa-B kinase subunit epsilon (IKKε) signaling by targeting IKBKE-e is an actionable strategy to elicit synthetic anticancer immunity in immunologically “cold” cancers such as prostate cancer.
Authors
Xiang Li, Rui Sun, Hao Li, Jacob J. Orme, Xu Zhang, Yu Hou, Sean S. Park, Yu Zhang, Yi He, Liguo Wang, Veronica Rodriguez-Bravo, Josep Domingo-Domenech, Shancheng Ren, Dan Xia, Guanghou Fu, Zhankui Jia, Haojie Huang
Abstract
Myelodysplastic syndromes (MDSs) are malignant hematopoietic stem and progenitor cell (HSPC) disorders that lead to ineffective blood production with poor outcomes. We previously showed that F-box only protein 11 (FBXO11) is downregulated in MDS, and here we report how this event contributes to disease progression. Integration of multiomics data revealed that the SCF-FBXO11 complex regulates spliceosome and ribosome components in a nucleophosmin 1 (NPM1)-centric network. FBXO11 facilitates the ubiquitylation of NPM1, whereby deletion of FBXO11 results in the reorganization of NPM1 and a de-repression of alternative splicing. Label-free total quantitative proteomics demonstrated that the FBXO11-NPM1 interactome was markedly downregulated in cells from patients with CD34+ MDS. In addition, we discovered that MYC was evicted from the FBXO11 promoter by TLR2 activation, revealing that it was a MYC target gene and explaining why FBXO11 expression was decreased in MDS. In MDS mouse models, genetic ablation of Fbxo11 exacerbated neutropenia concomitant with a profound decrease in NPM1 protein levels. Finally, we discovered rare mutations in FBXO11, which mapped to a previously unstudied functional intrinsically disordered region (IDR) in the N-terminus responsible for binding NPM1. These data support a model in which FBXO11 rewires RNA binding and ribosomal subnetworks through ubiquitylation of NPM1, ultimately restricting MDS progression.
Authors
Madeline Niederkorn, Lavanya Bezavada, Anitria Cotton, Lance E. Palmer, Lahiri Konada, Trent Hall, Vishwajeeth R. Pagala, Jinbin Zhai, Zuo-Fei Yuan, Yingxue Fu, Jacob A. Steele, Shilpa Narina, Andrew Schild, Chengzhou Wu, Sarah Aminov, Michael Schieber, Erin McGovern, Aaron B. Taylor, Sandeep Gurbuxani, Peng Xu, Peng Ji, Laura J. Janke, Anthony A. High, Guolian Kang, Shondra M. Pruett-Miller, Mitchell Weiss, Amit Verma, Raajit K. Rampal, John D. Crispino
Abstract
Despite overexpression of N-acetyltransferase 10 (NAT10) in colorectal cancer (CRC), its immunomodulatory role in the tumor microenvironment remains elusive. Here, we reveal that NAT10 promotes immune evasion through N4-acetylcytosine–dependent (ac4C-dependent) mRNA stabilization. Using syngeneic mouse models (MC38/CT-26), intestinal epithelial-cell specific Nat10 conditional KO (Nat10cKO) mice, patient-derived organoids, and clinical specimens, we show that Nat10 ablation enhanced CD8+ T cell–mediated antitumor immunity. Single-cell RNA-seq revealed increased cytotoxic CD8+ T cell infiltration in Nat10cKO tumors, which was corroborated by the inverse correlation of tumoral NAT10 expression and CD8+ T cell number in clinical specimens. Multi-omics integration analysis identified DKK2 as the predominant NAT10-regulated transcript. NAT10 stabilized DKK2 mRNA via ac4C modification, leading to high expression of the DKK2 protein. Secreted DKK2 engaged LRP6 receptors to activate AKT-mTOR signaling, inducing cholesterol accumulation in CD8+ T cells and impairing their cytotoxicity. Pharmacological NAT10 inhibition (Remodelin treatment) or DKK2 neutralization restored CD8+ T cell function and synergized with anti–PD-1 therapy. Our findings establish the NAT10/DKK2/LRP6/AKT-mTOR/cholesterol axis as a critical regulator of CD8+ T cell dysfunction in CRC, positioning NAT10/DKK2 as a potential target to enhance immunotherapy efficacy.
Authors
Mengmeng Li, Xiaoya Zhao, Jun Wu, Shimeng Zhou, Yao Fu, Chen Chen, Zhuang Ma, Jiawen Xu, Yun Qian, Zhangding Wang, Bo Wang, Qiang Wang, Qingqing Ding, Changyu Chen, Honggang Wang, Xiaozhong Yang, Weijie Dai, Wenjie Zhang, Shouyu Wang
Abstract
Mutation-associated neoantigens (MANAs) are highly cancer-specific targets for immunotherapy where peptides derived from intracellular mutant proteins are presented on the cell surface via HLA molecules. T cell–engaging bispecific antibodies and CAR T cells can target MANAs to eliminate cancer cells via T cell activation. However, the low antigen density of MANAs on the cell surface can limit therapeutic efficacy. Here, we investigated whether increasing the affinity of the H2 single-chain variable fragment (scFv) targeting the p53 R175H MANA (HMTEVVRHC presented on HLA-A*02:01) improves its therapeutic effect. We identified higher-affinity H2 variants via phage biopanning and a thiocyanate elution method. Increasing bispecific antibody affinity to the low nanomolar range increased cancer cell killing and tumor control in mouse xenograft models without sacrificing antigen specificity. We next asked how increasing scFv affinity impacts CAR T cell function — a matter of debate. We appended each variant scFv to a CD28z CAR, CD3γ, or the T cell receptor. In striking contrast to the bispecific antibody results, increasing CAR affinity decreased function in each CAR format due to lower T cell activation upon interaction with target cancer cells. These results have important implications for the design of future immunotherapeutic approaches targeting low-density antigens.
Authors
Sarah R. DiNapoli, Katharine M. Wright, Brian J. Mog, Alexander H. Pearlman, Tushar D. Nichakawade, Nikita Marcou, Emily Han-Chung Hsiue, Michael S. Hwang, Jacqueline Douglass, Qiang Liu, Evangeline Watson, Marco Dal Molin, Joshua D. Cohen, Maria Popoli, Suman Paul, Maximilian F. Konig, Nicolas Wyhs, P. Aitana Azurmendi, Stephanie Glavaris, Jiaxin Ge, Tolulope O. Awosika, Jin Liu, Kathleen L. Gabrielson, Sandra B. Gabelli, Drew M. Pardoll, Chetan Bettegowda, Nickolas Papadopoulos, Kenneth W. Kinzler, Shibin Zhou, Bert Vogelstein
Abstract
Epidermal growth factor receptor (EGFR)-activating mutations are established biomarkers of resistance to immune checkpoint blockade (ICB) in lung cancer, yet the precise molecular mechanism and effective therapeutic strategies remain elusive. In this study, we show that EGFR overexpression and amplification recapitulate the negative impact of EGFR driver mutations to ICB response, indicating a proactive involvement of EGFR signaling in antagonizing antitumor immune response. Functional studies unveil that EGFR activation suppresses cellular response to interferon-gamma (IFN-γ) following ICB treatment across multiple cancer models. This impairment in IFN-γ responsiveness further limits the upregulation of T cell-recruiting chemokines and antigen presentation, resulting in reduced T cell infiltration and activation, ultimately undermining antitumor immunity. Mechanistically, EGFR promotes SHP2 activation to accelerate STAT1 dephosphorylation, leading to premature termination of the IFN-γ response. SHP2 inhibition restored ICB sensitivity in EGFR-activated tumors, significantly reducing tumor burden while maintaining a favorable safety profile. Our findings suggest that EGFR/SHP2 axis functions as a molecular brake to disrupt the initiation and amplification of IFN-γ mediated anti-tumor response during immunotherapy. This discovery unveils a potential avenue to overcome immunotherapy resistance in EGFR-driven tumors, particularly lung cancer, through SHP2-targeted combination strategies.
Authors
Wei-Tao Zhuang, Lan-Lan Pang, Li-Yang Hu, Jun Liao, Jian-Hua Zhan, Ting Li, Ri-Xin Chen, Jia-Ni Zheng, An-Lin Li, Wen-Yan Yu, Tian-Qin Mao, Liang Chen, Yu-Jian Huang, Shao-Dong Hong, Jing Li, Jun-Han Wu, Yi-Ming Zeng, Meng-Juan Yang, Hai-Qing Zeng, Ya-Xiong Zhang, Li Zhang, Wen-Feng Fang



Copyright © 2026 American Society for Clinical Investigation
ISSN: 0021-9738 (print), 1558-8238 (online)